
Surgeons are debating the role of cyclophotocoagulation (CPC) in glaucoma management. Some ophthalmologists view the procedure exclusively as a treatment option for painful and/or poorly sighted eyes. Others believe that CPC can be used earlier in the disease process and in sighted eyes. The latter perspective is motivated in part by variations on the original transscleral CPC approach such as the slow coagulation technique proposed by Gaasterland.1 Further spurring interest in CPC are relatively recent improvements in laser delivery probes using MicroPulse technology (Iridex; Figure 1).
AT A GLANCE
• According to Dr. Fox, the view of transscleral cyclophotocoagulation as a last-ditch treatment for refractory glaucoma typically derives from complications documented in early studies and reports.
• Sufficient evidence exists to encourage ophthalmologists to consider using this repeatable noninvasive glaucoma intervention in a wider range of patients, says Dr. Fox.
• Dr. Brubaker counters that the biggest challenge in justifying the use of transscleral cyclophotocoagulation in sighted eyes with good vision is the real risk of vision loss.
ADVANTAGES
Clinical advantages of CPC compared with other surgical interventions for glaucoma include an ability to titrate energy settings, which allows surgeons to customize treatment to the individual patient. Iris pigmentation, a relative indicator of ciliary body pigmentation, can help surgeons determine the proper energy settings for any given treatment.1 Postoperative restrictions are nonexistent, and the burden of postoperative visits tends to be less than with traditional glaucoma surgical approaches. With lower energy settings, it is less likely that CPC will lead to conjunctival scarring, leaving the vast majority of patients candidates for further surgical intervention involving the conjunctiva, should it be needed. Anesthesia can be achieved via a retrobulbar block and/or conscious sedation. CPC also provides logistical flexibility, because the procedure may be performed in either an office or an OR setting.
A major advantage of CPC is that it can be repeated if the first treatment does not yield the desired result. Surgeons thus have greater flexibility in using nondestructive or less destructive (MicroPulse or slow-coagulation) settings for initial applications, because energy levels can be modified for repeat treatments. In my experience, this flexibility has allowed initial CPC to be relatively low risk, with subsequent treatments titrated to have more effect if needed in the cases that are initially refractory to CPC.
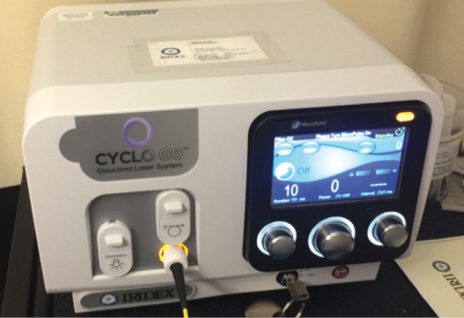
Figure 1. Cyclo G6 Glaucoma Laser System (Iridex).
WHY THE CONCERN?
The view of CPC as a last-ditch treatment for refractory glaucoma typically derives from complications documented in early studies and reports. Loss of vision can result from cataract formation, cystoid macular edema, ocular surface issues related to neurotrophic corneal effects, hypotony, or chronic inflammatory effects such as choroidal effusions. Add to this the risk of chronic pain, an atonic pupil, phthisis, and even sympathetic ophthalmia, and it is no wonder some surgeons are leery of CPC.

Figure 2. Proper positioning of the MP3 probe, with the notch (red arrow) toward the limbus and the flat side (blue arrow) toward the eyelid.
Although the potential for these complications exists, follow-up studies have demonstrated that vision loss after CPC may have more to do with the advanced stage of disease and with glaucomatous progression than with the treatment modality itself.2 CPC using the traditional G-probe relies on three variables related to the laser itself: the power of the laser, the duration of laser application, and the number of treatment spots. The energy of the treatment is a function of the power and duration of the laser administered. Spreading lower power over a longer duration (ie, slow coagulation) has shown promise for minimizing complications.1 The rate of complications also tends to be related to the total energy used in a treatment session.3 Several studies investigating the use of CPC in sighted eyes have reported promising results.2,4-6 These findings tend to be limited by the retrospective study design but should be respected for what they are: at worst, they warrant further investigation, and at best, the review of more recent studies may prompt surgeons to consider using CPC in a wider range of patients.
THE PROBE MATTERS
In sighted eyes, performing CPC with MicroPulse technology seems to be less controversial than using the traditional G-probe. Approved by the FDA in 2015, the MicroPulse P3 probe (MP3 probe; Iridex; Figure 2) transsclerally delivers noncontinuous 810-nm laser treatment to the pigmented ciliary body epithelium, with the energy distributed to the aqueous-producing nonpigmented ciliary body epithelium. The surgeon performs a sweeping movement along the limbus, excluding the 2:30- to 3:30- and the 8:30- to 9:30-o’clock positions, as opposed to spot application with the G-probe. The three variables of treatment with the MP3 probe are duty cycle (percentage of time the laser is administering energy), laser power, and total treatment duration. The noncontinuous nature of the MicroPulse therapy decreases aqueous production without destroying the targeted tissues,7 unlike the traditional G-probe’s continuous delivery of laser energy, which leads to focal destruction. This difference leads to a reduced inflammatory response to MicroPulse treatment.
MicroPulse CPC has favorable efficacy and complication profiles.8,9 Anecdotally, surgeons using the MP3 probe have reported an improvement in postoperative inflammation and pain compared with the G-probe, and this has been demonstrated in the literature.9 These benefits combined with fewer complications lead to a more predictable postoperative course for both patients and surgeons. The safety profile also suggests that MicroPulse CPC could be used earlier in the disease process and in eyes that have a better visual prognosis.
CONCLUSION
Further research will likely influence the future role of CPC in glaucoma management. Long-term studies of MicroPulse CPC are needed. A review of current CPC studies shows wide variation in the laser power and duration used. Further investigations that compare varying energy/duration with the use of the G-probe would also help surgeons determine the best balance between safety and efficacy. Varying energy/duty cycles with the use of the MP3 probe may also be worth evaluating.
CPC may never achieve the refined sophistication that phacoemulsification has today, but it is worth remembering that the latter procedure was barbaric in its original form compared to its current iteration. The evolution of glaucoma surgery is leading to earlier intervention in the disease process with the development of microinvasive techniques and devices. As a repeatable noninvasive glaucoma intervention, CPC deserves another look by surgeons who have categorized it as a treatment option for refractory glaucoma in poorly sighted eyes only. Varying technique and the use of different laser delivery platforms have been shown to have a safety profile that is distinct from the highly destructive CPC treatments of the past. Sufficient evidence exists to lead ophthalmologists and glaucoma subspecialists to consider using CPC in a wider range of patients.
Counterpoint
By Jacob Brubaker, MD

The safety of transscleral cyclophotocoagulation (TSCPC) has recently improved. The improved G-probe and MicroPulse technology (Iridex) offer the promise of better outcomes with reduced risk. A procedure once deemed useful only for treating eyes with poor visual potential and the most recalcitrant glaucoma is now finding wider acceptance for the management of earlier, milder forms of the disease. Some ophthalmologists have even advocated offering TSCPC as a potential first-line procedure for patients with good vision. Although the safety profile of TSCPC has improved, I still feel that moving the procedure up in the traditional glaucoma treatment paradigm carries risks that should be clear to the patient and the surgeon. Reasons to avoid using TSCPC as an early treatment option include the risk of developing chronic uveitis, loss of vision, cataract formation, and conjunctival scarring. These risks and the advent of other safer, more effective glaucoma procedures make it difficult for me to advocate the early application of TSCPC.
The biggest challenge in justifying the use of TSCPC in sighted eyes with good vision is the real risk of vision loss. Studies looking at treatment in sighted eyes show a loss of vision in 20% to 30% of patients.1,2 Although some ophthalmologists have argued that this statistic is similar to that for other traditional glaucoma procedures, including trabeculectomy or drainage devices, I find that vision loss from TSCPC tends to be more severe and drastic. Vision loss associated with incisional surgeries is often caused by specific, treatable causes such as hypotony from overfiltration; although it may require a second procedure, vision is often recoverable. In contrast, the vision loss from TSCPC is often intractable or unexplained. Causes include macular edema, phthisis, and hypotony due to aqueous shutdown—all challenging if not impossible to treat.
Although I feel that TSCPC should not be used too early in the glaucoma treatment paradigm, I am nonetheless a firm believer in the procedure’s utility. I think it offers great benefit in patients with poor visual potential or those who are poor candidates for incisional surgery. I typically follow the American Academy of Ophthalmology’s guidelines, which state that “cyclophotocoagulation is indicated for patients with refractory glaucoma who have failed trabeculectomy or tube shunt procedures, patients with minimal useful vision and elevated IOP, patients who have no visual potential and need pain relief, and patients with complicated glaucoma and conjunctival scarring from previous surgery. It may be useful for patients whose general medical condition precludes invasive surgery or who refuse more aggressive surgery.”3 I routinely offer TSCPC to patients who retain good vision but have undergone multiple surgeries. In these cases, I feel that the risks of additional incisional surgery coupled with its low likelihood of success are enough to favor TSCPC. I often find that TSCPC is the treatment option that finally works.
Even though the complication is less common with modern TSCPC technology, vision loss unfortunately occurs in some cases. It helps patients and surgeons to know at that point that all other treatment options were exhausted. I hope such outcomes become even rarer with the further development of more minimally invasive glaucoma surgeries and the safer, earlier treatment of disease.
1. Egbert PR, Fladoyor S, Budenz DL, et al. Diode laser transscleral cyclophotocoagulation as a primary surgical treatment for primary open-angle glaucoma. Arch Ophthalmol. 2001;119:345-350.
2. Pokroy R, Greenwald Y, Pollack A, et al. Visual loss after diode laser cyclophotocoagulation for primary open-angle glaucoma and neovascular glaucoma. Ophthalmic Surg Lasers Imaging. 2008;39(1):22-29.
3. Pastor SA, Singh K, Lee DA, et al. Cyclophotocoagulation: a report by the American Academy of Ophthalmology. Ophthalmology. 2001;108(11):2130-2138.
Jacob Brubaker, MD
• glaucoma and anterior segment surgery, Sacramento Eye Consultants, Sacramento, California
• (916) 649-1515; jbrubaker@saceye.com
• financial interest: none acknowledged
1. Gaasterland DE. Diode laser cyclophotocoagulation. Glaucoma Today. March 2009;7(2):35-37,41.
2. Egbert PR, Fiadoyor S, Budenz DL, et al. Diode laser transscleral cyclophotocoagulation as a primary surgical treatment for primary open-angle glaucoma. Arch Ophthalmol. 2001;119:345-350.
3. Aujla JS, Lee GA, Vincent SJ, et al. Incidence of hypotony and sympathetic ophthalmia following trans-scleral cyclophotocoagulation for glaucoma and a report of risk factors. Clin Exp Ophthalmol. 2013;41(8):761-772.
4. Rotchford AP, Jayasawal R, Madhusudhan S, et al. Transscleral diode laser cycloablation in patients with good vision. Br J Ophthalmol. 2010;94(9):1180-1183.
5. Ansari E, Gandhewar J. Long-term efficacy and visual acuity following transscleral diode laser photocoagulation in cases of refractory and non-refractory glaucoma. Eye. 2007;21:936-940.
6. Bleisch D, Furrer S, Funk J. Rates of glaucomatous visual field change before and after transscleral cyclophotocoagulation: a retrospective case series. BMC Ophthalmol. 2015;15:179.
7. Noecker R. Glaucoma treatment for today... & tomorrow. Iridex. https://www.youtube.com/watch?v=qf05g3Ob8ds. Published April 14, 2015. Accessed March 6, 2017.
8. Aquino MCD. Micropulse versus continuous wave transscleral diode cyclophotocoagulation in refractory glaucoma: a randomized exploratory study. Clin Experiment Ophthalmol. 2015;43(1):40-46.
9. Tan A, Chockalingam M, Aquino M, et al. Micropulse transscleral diode laser cyclophotocoagulation in the treatment of refractory glaucoma. Clin Experiment Ophthalmol. 2010;38(3):266-272.
James Fox, MD
• glaucoma and advanced anterior segment surgery, Icon Eye Care, Grand Junction, Colorado
• (970) 256-0400; jafox1981@gmail.com
• financial interest: none acknowledged
