The COVID-19 crisis has emphasized the importance of the ability to adapt to changing times by working smarter and more safely. In glaucoma specifically, we have seen quick adjustments made to IOP exams, with some offices implementing drive-through pressure checks. We saw a substantial increase in telehealth visits and began to connect routinely with patients in a way we likely had never dreamed. Even mainstay methods such as visual field tests shifted dramatically toward safer and easier-to-clean modalities (eg, virtual reality headsets) and away from the classic white-on-white automated perimetry conducted in bowls. The year 2020 also taught us that cultural awareness goes beyond what was considered the norm in years past. As society becomes more culturally aware, it may be time to rethink eye exams.
We conducted an informal survey at my office in the Bronx, New York, in which we asked approximately 300 patients about a range of elements of their eye exam experience. As expected, most patients commented on social distancing in the office, and some did not appreciate the wait times. These mutable elements are more a function of staffing and scheduling—constant disruptors in the office. We were surprised, however, by the responses regarding issues with the slit-lamp exam. Patients cited challenges with head positioning, mask wearing, and chest compression. These complaints were significant enough to negatively affect about 10% of the patients surveyed.
MASK ISSUES
For most of the COVID-19 pandemic, masks have been mandatory in New York City businesses. Although some restrictions were recently lifted, indoor mask wearing is still recommended for vaccinated individuals and required for unvaccinated individuals.
Masks with pronounced protuberances may interfere with proper positioning of the Goldmann tonometer and may result in faulty readings (Figure 1). These masks include cupped N95 masks, duck-billed KN95 masks, silicone-supported fabric masks, and standard surgical masks with poorly positioned metal nasal molds. The challenges occur mainly owing to the greater dimensions of these masks compared with standard surgical masks and because of a preshaped rigid nose area that may press against the Goldmann tonometer.1

Figure 1. Masks with pronounced protuberances may interfere with proper positioning of the Goldmann tonometer and may result in faulty readings.
Recommendations for curtailing these issues include the following:
- Adjust the patient’s mask to the side while covering their nose and mouth if possible;
- Tilt the patient’s head slightly away from the tonometer arm to clear the feeder arm while asking the patient to maintain a forward gaze;
- Compress the patient’s mask with your hand or a cotton-tipped applicator to prevent any contact during measurement; and
- If none of these adjustments is successful, consider using a handheld tonometer, such as the iCare IC100 (iCare USA) or Tono-Pen (Reichert Technologies).2
Despite the use of these tactics, it still may be necessary for patients to remove their masks during IOP measurement. This places the examiner and the patient at risk of airborne pathogen exposure. With mask wearing’s likely becoming a long-term scenario as new COVID strains emerge, device manufacturers may benefit from tonometer redesigns that eliminate this safety burden. A design similar to that of the AT 870 applanation tonometer (Haag-Streit; Figure 2), which does not come in contact with the lower portion of the patient’s face, is worth exploring.

Figure 2. The AT 870 applanation tonometer does not come in contact with the lower portion of the patient’s face, making the device mask-friendly.
CHEST DISCOMFORT
From 1999 to 2018, the age-adjusted prevalence of obesity increased from 30.5% to 42.4%, and the prevalence of severe obesity increased from 4.7% to 9.2%.3 In an ophthalmic practice, obesity affects how patients are examined with the current slit lamp designs. Obese patients, women in particular, are most likely to be physically restricted from properly fitting into the slit-lamp headrest, mainly because of increased upper chest circumference (Figure 3). In this scenario, the focus of the anterior segment exam is affected, Goldmann applanation tonometry is not possible, and patients experience significant chest pressure and discomfort. Some newer fundus cameras such as the Eidon (Centervue; Figure 4) have an offset headrest design to minimize discomfort for obese and, in particular, female patients.
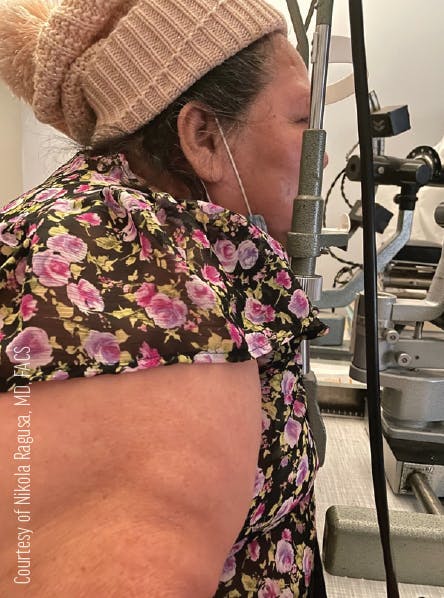
Figure 3. Obese patients (women in particular) may be physically restricted from properly fitting into the head rest of most slit lamps because of increased upper chest circumference.
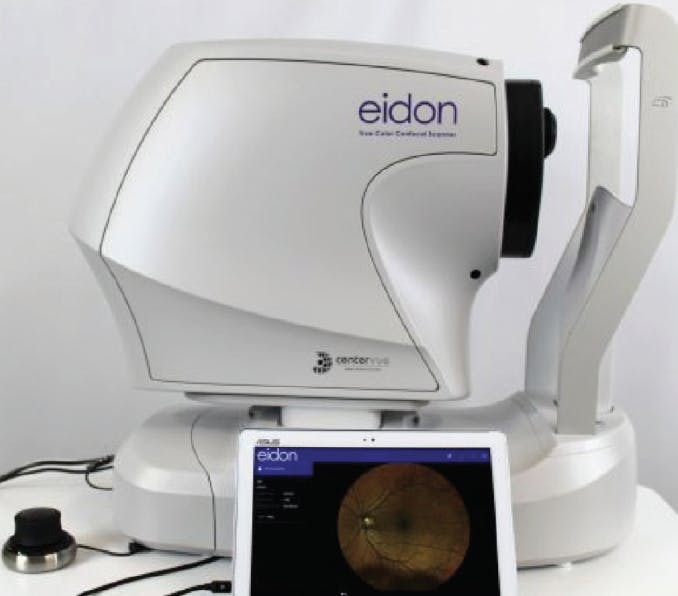
Figure 4. The Eidon fundus camera features an offset headrest design to minimize patient discomfort.
HEAD POSITIONing
Another element of the exam that patients in my office rated negatively was the physical positioning of their head in the slit lamp. This issue affected individuals who wear head coverings or have hairstyles that alter the height and width of their head in the slit lamp. These patients were not able to fit into the typical closed-loop slit-lamp head holder. An open and wider headrest design would be more culturally appropriate and would make the exam more comfortable for these patients.
CONCLUSION
The Haag-Streit 900 has long been the gold standard in slit-lamp design. Introduced in 1958, this device has become the most copied and respected style of slit lamp on the eye care market. Although this device provides excellent optics and comfort for the eye care provider, the patient’s experience may require more attention and innovation.
The past several decades have brought great cultural and social changes, and this evolution has affected the practice of medicine and attitudes toward patients’ comfort. In addition to taking physicians’ preferences into account, it may be time for all device manufacturers to consider how patients feel about their exams. In our practice survey, patients who could not fit into the slit-lamp headrest reported feeling embarrassed, uncomfortable, ashamed, body-conscious, out of breath from chest compression, and upset. As we become more culturally sensitive as a society, we must recognize that the design of our ophthalmic equipment may not be accessible to all patients and may therefore warrant rethinking.
1. Quaranta L, Micheletti E, Riva I, Weinreb RN. Intraocular pressure measurement in patients wearing filtering facepiece masks. J Glaucoma. 2020;29(10)999-1000.
2. St. Peter D, Seibold L, Kahook MY. The effect of mask wearing on reliability of Goldmann applanation tonometry. Glaucoma Physician. December 1, 2020. Accessed July 1, 2020. www.glaucomaphysician.net/issues/2020/december-2020/web-exclusive-the-effect-of-mask-wearing-on-reliab
3. Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity and severe obesity among adults: United States, 2017–2018. CDC. February 2020. Accessed July 1, 2021. https://www.cdc.gov/nchs/products/databriefs/db360.htm



