Vascular factors have been suggested to influence the development and progression of glaucoma, and they are thought to be especially relevant for patients with normal-tension glaucoma (NTG). As part of the Leuven Eye Study, we sought to determine which vascular factors better described patients with NTG compared to those with primary open-angle glaucoma (POAG).1
THE INVESTIGATION
A total of 384 patients from the Leuven Eye Study (182 with NTG and 202 with POAG) were included in our investigation. We used this database to compute three multivariate logistic regression models, including (1) a conventional model (conventional variables only, including vascular-related self-reported phenomena*); (2) an advanced vascular model (advanced vascular parameters only: color Doppler imaging [CDI], retinal oximetry, ocular pulse amplitude, and choroidal thickness); and (3) a global model, in which both types of parameters were allowed. Receiver operating characteristic curves and corresponding areas under the curve (AUCs) were calculated and compared between models.
We found that patients with NTG had a higher resistive index (Figure) and lower early systolic acceleration in their retrobulbar vessels on CDI and a smaller arteriovenous retinal oxygen saturation difference on retinal oximetry. The global model (AUC 0.743) showed a significantly better discriminative ability than the conventional model (AUC 0.687, P = .049) or the advanced vascular model (AUC 0.677, P = .005). The conventional and advanced vascular models showed a similar discriminative ability (P = .0823).
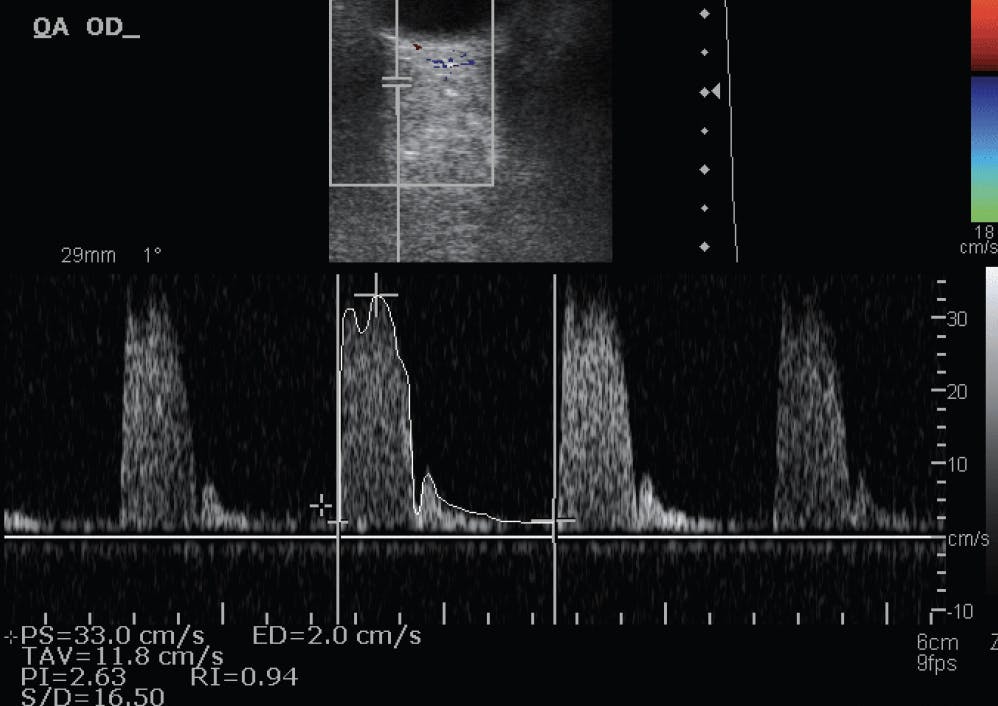
Figure. CDI of the ophthalmic artery of a patient with NTG in the Leuven Eye Study. There is a considerably high resistive index, which can be one of the many factors responsible for glaucomatous progression.
Conclusions and Future Directions
Patients with NTG have more signs of vascular dysfunction than those with POAG. Clinical conventional parameters, such as asking simple vascular-related questions, combined with advanced vascular examinations may help to better elucidate the role that non–IOP-related factors play in NTG. Nonetheless, the aforementioned advanced vascular techniques are neither widely available nor easy to perform.
Further evaluations of the Leuven Eye Study cohort have been conducted, and new publications are expected soon. These will include new data retrieved with OCT angiography and a retinal dynamic vessel analyzer (DVA 3.0, Imedos Health), which were not available when the study started. Nonetheless, regarding OCT angiography, certain breakthroughs are still needed, among which are the incorporation of automatic vessel density quantification software in all devices and the ability to adjust for certain confounders, such as age, scan quality, axial length, and blood pressure. The future of advanced vascular analysis in glaucoma is bright, but further developments are needed for implementation into routine clinical care.
*Conventional parameters include age, sex, IOP and IOP-lowering medication, central corneal thickness, cup-to-disc ratio, structural optic nerve parameters, visual acuity, visual field parameters, blood pressure and blood pressure–lowering medication, migraine, and self-reported peripheral vasospam.
1. Barbosa-Breda J, Keer KV, Abegão-Pinto L, et al. Improved discrimination between normal-tension and primary open-angle glaucoma with advanced vascular examinations - the Leuven Eye Study. Acta Ophthalmol. 2019;97(1):e50-e56.






